Actinic Keratosis
Individuals with fair complexions are at a significantly higher risk for developing Actinic Keratosis. This includes those with light skin tones, blonde or red hair, and blue or green eyes. The natural lack of melanin in their skin offers less protection against harmful UV radiation. Additionally, people who have spent a significant portion of their lives outdoors, whether due to occupational exposure or recreational activities, are more prone to this condition. The risk accumulates over time, meaning the more sun exposure one has, the greater the likelihood of developing these lesions.
Actinic Keratosis is most commonly diagnosed in individuals aged forty and older. As we age, our skin's ability to repair UV radiation damage diminishes, leading to the appearance of these lesions. However, younger individuals with significant sun exposure can also develop Actinic Keratosis.
Recognizing and treating Actinic Keratosis is crucial because it is considered a precancerous condition. If left untreated, these lesions can potentially progress to squamous cell carcinoma, a type of skin cancer.
Regular skin examinations by a dermatologist are vital for managing Actinic Keratosis. At Lupton Dermatology in Greensboro, our skin experts are trained to identify and treat these lesions early, reducing the risk of progression to more severe conditions. Given its potential to progress to skin cancer, prompt and effective treatment is essential.
Examples Actinic-Keratosis
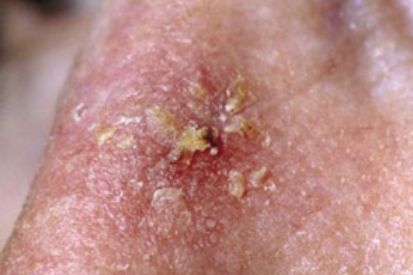
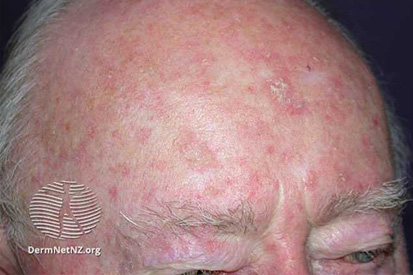
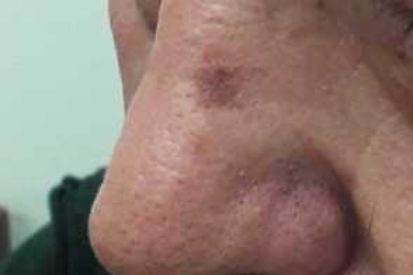
What are the Symptoms of Actinic Keratosis?
- Actinic Keratosis can reach a quarter of an inch in size and may even disappear for a time.
- May appear red, light or dark tan, pink or skin-colored.
- These patches may be sensitive or tender and may become inflamed or even bleed.
- Although the patches are typically dry they may also present as lesions that do not heal or as thick, horny growths.
Causes of Actinic Keratosis
- Actinic keratosis (AK) is primarily caused by prolonged exposure to ultraviolet (UV) radiation from the sun or artificial sources like tanning beds.
- The cumulative effect of sun damage leads to the development of these precancerous lesions.
- The risk of actinic keratosis increases with age, reflecting the cumulative impact of sun exposure over the years.
- Individuals with weakened immune systems may be at a higher risk of developing actinic keratosis.
How to Prevent Actinic Keratosis
- Sunscreen: Regularly apply a broad-spectrum sunscreen with a high SPF to exposed skin, even on cloudy days. Reapply every two hours and more frequently if sweating or swimming.
- Protective Clothing: Wear protective clothing, such as wide-brimmed hats, long sleeves, and sunglasses, to shield the skin from direct sunlight. Clothing with a tight weave offers additional protection.
- Seek Shade: Limit direct sun exposure during peak hours, typically between 10 a.m. and 4 p.m. When outdoors, seek shade under trees, umbrellas, or other structures.
- Avoid Tanning Beds: Refrain from using tanning beds, as they emit harmful UV radiation that contributes to skin damage.
- Regular Skin Examinations: Perform at-home self-examinations of the skin regularly to detect any changes or new lesions as well as schedule annual total body skin exams with your trusted dermatology provider. Notify your provider of any suspicious growths or changes you find.
- Limit Alcohol and Tobacco: Excessive alcohol consumption and smoking can contribute to skin damage, so moderation or cessation of these habits is beneficial.
- Stay Hydrated: Proper hydration helps maintain skin health. Drink an adequate amount of water to support overall skin function.
Actinic Keratosis FAQs
Actinic Keratosis (AK) lesions are generally not painful, which can make them easy to overlook. Many individuals with AK may not experience any significant discomfort. The lesions often present as rough, scaly patches on the skin that may feel slightly raised. Despite the absence of pain, these lesions can be noticeable due to their texture and appearance.
However, some people might experience mild symptoms associated with Actinic Keratosis. These can include tenderness, itching, or a slight burning sensation in the affected areas. The degree of discomfort can vary from person to person, with some experiencing more pronounced sensations than others. These symptoms might be intermittent or persist over time, depending on the extent and location of the lesions.
It is important to monitor any changes in your skin closely. While AK lesions are typically not a source of severe pain, any new or evolving symptoms, such as increased tenderness, significant itching, or a burning sensation, should not be ignored. These changes could indicate irritation or the potential progression of the lesions, which warrants medical attention.
If you notice any new lesions or changes in existing ones, it is crucial to consult with a dermatologist. Dermatologists are specialists in diagnosing and managing skin conditions, including Actinic Keratosis. They can perform a thorough evaluation of your skin to determine the nature of the lesions and recommend appropriate treatment options. Early detection and intervention are key to preventing AK from progressing to more serious conditions, such as squamous cell carcinoma.
In addition to professional medical evaluation, there are preventive measures you can take to protect your skin from further damage. Using broad-spectrum sunscreen with a high SPF, wearing protective clothing, and avoiding peak sun exposure hours are effective strategies to reduce the risk of developing additional Actinic Keratosis lesions.
While Actinic Keratosis lesions are typically not painful, some individuals may experience mild symptoms such as tenderness, itching, or a burning sensation. It is important to remain vigilant about any changes in your skin and seek prompt evaluation from a dermatologist if you have concerns. Regular skin check-ups and protective measures can help manage and prevent Actinic Keratosis, ensuring better skin health over the long term.
Actinic Keratosis (AK) typically does not resolve on its own. These lesions, which result from long-term sun exposure, are considered precancerous and have the potential to progress to squamous cell carcinoma (SCC), a type of skin cancer. Consequently, it's crucial to address AK promptly to prevent more serious health issues.
Without treatment, Actinic Keratosis lesions can persist and even worsen over time. The risk of progression to SCC varies, but given the potential severity, it is essential not to ignore these lesions. The transition from AK to SCC involves the lesion becoming thicker, more tender, and possibly developing into an open sore. This progression underscores the importance of medical intervention.
If you suspect you have Actinic Keratosis, seeking medical attention from a dermatologist is imperative. Dermatologists are trained to diagnose and treat skin conditions like AK. During a consultation, a dermatologist will assess the lesions to confirm the diagnosis. This assessment may involve a visual examination and, in some cases, a biopsy to determine if the lesion has started to progress towards cancer.
Once diagnosed, several treatment options are available to manage Actinic Keratosis effectively. Common treatments include:
- Cryotherapy: This method involves freezing the lesion with liquid nitrogen, causing it to peel away.
- Topical Medications: Creams and gels such as 5-fluorouracil, imiquimod, or diclofenac can be applied to the lesions to treat them.
- Photodynamic Therapy (PDT): This treatment uses a photosensitizing agent applied to the skin, followed by exposure to a specific type of light to destroy the abnormal cells.
- Chemical Peels: Strong acids are used to peel away the top layer of skin, removing the lesions.
- Laser Therapy: Intense light beams are used to target and remove the affected skin.
In addition to these treatments, your dermatologist will also provide guidance on preventive measures to protect your skin from further damage. This includes the use of broad-spectrum sunscreens with a high SPF, wearing protective clothing, and avoiding sun exposure during peak hours.
Regular follow-up appointments with your dermatologist are vital. These visits allow for ongoing monitoring of your skin to catch any new lesions early and to ensure that treated lesions do not recur or progress. Early detection and treatment are key to managing Actinic Keratosis effectively and preventing its progression to skin cancer.
Actinic Keratosis does not typically go away on its own and requires medical attention. Without treatment, these precancerous lesions can develop into squamous cell carcinoma. Consulting a dermatologist for assessment, treatment, and regular monitoring is crucial for managing Actinic Keratosis and maintaining healthy skin.
Diagnosing Actinic Keratosis (AK) is a crucial step in managing and treating this precancerous condition. Dermatologists, who are experts in skin health, employ several methods to accurately identify AK lesions.
The primary method for diagnosing Actinic Keratosis is through a thorough visual examination of the skin. During this examination, the dermatologist carefully inspects the skin for any rough, scaly patches or lesions that are characteristic of AK. These lesions often appear on sun-exposed areas of the body, such as the face, ears, neck, forearms, and the backs of the hands. Dermatologists use their trained eyes and sometimes magnifying tools to assess the texture, color, and size of the lesions.
In some instances, a visual examination may not provide enough information to make a definitive diagnosis. When there is uncertainty, or if the lesion has atypical features, the dermatologist may perform a skin biopsy. A biopsy involves removing a small sample of the affected skin, which is then sent to a laboratory for detailed analysis. The laboratory examination can confirm whether the lesion is indeed Actinic Keratosis or if it is another type of skin condition, including skin cancer such as squamous cell carcinoma or basal cell carcinoma.
The biopsy procedure is typically straightforward and performed under local anesthesia to minimize discomfort. The dermatologist cleans the area, numbs it with an anesthetic, and then uses a small, sharp instrument to remove a portion of the lesion. After the sample is taken, the site may be covered with a bandage, and the patient may receive instructions on how to care for the biopsy site as it heals.
Laboratory analysis of the biopsy sample involves examining the tissue under a microscope. Pathologists, who specialize in diagnosing diseases by studying cells and tissues, look for specific cellular changes that indicate Actinic Keratosis or other skin conditions. This detailed examination helps ensure an accurate diagnosis, which is critical for determining the appropriate treatment plan.
In addition to visual examination and biopsy, dermatologists may use dermoscopy, a non-invasive diagnostic tool that provides a magnified view of the skin. Dermoscopy can help dermatologists see patterns and structures in the skin that are not visible to the naked eye, aiding in the differentiation of Actinic Keratosis from other skin lesions.
Regular skin checks and monitoring are essential, especially for individuals at higher risk of developing Actinic Keratosis. These include people with fair skin, those who have had significant sun exposure, and older adults. Early detection and diagnosis allow for timely intervention, which can prevent the progression of AK to more serious conditions like squamous cell carcinoma.
Actinic Keratosis is primarily diagnosed through a visual examination by a dermatologist. When necessary, a skin biopsy is performed to confirm the diagnosis and rule out skin cancer. This comprehensive approach ensures accurate diagnosis and effective management of the condition. Regular check-ups and skin monitoring are crucial for early detection and treatment, maintaining overall skin health.
You should apply sunscreen every single day, not just during sunny summer months. UV rays are present year-round and can penetrate clouds, causing skin damage even on overcast days. This means that sunscreen is necessary during winter, on cloudy days, and when spending time indoors near windows, as UV rays can pass through glass.
Before Sun Exposure
To ensure that sunscreen provides the best protection, it needs time to be properly absorbed into the skin. Therefore, you should apply sunscreen at least 15 to 30 minutes before going outside. This waiting period allows the sunscreen to form an effective barrier against UV rays.
Choosing the Right Sunscreen
For daily use, it’s recommended to choose a broad-spectrum sunscreen with an SPF (Sun Protection Factor) of at least 30. Broad-spectrum sunscreens protect against both UVA and UVB rays, which are responsible for skin aging and burning, respectively.
Reapplication
Sunscreen’s effectiveness diminishes over time, especially when exposed to sweat, water, or after toweling off. It is crucial to reapply sunscreen every two hours when you are outdoors. If you are swimming or sweating, reapply more frequently, following the instructions on the product label. Water-resistant sunscreens are available, but even these need to be reapplied after swimming or excessive sweating.
Proper Application
Ensure you apply sunscreen generously to all exposed skin. Most adults need about one ounce (approximately a shot glass full) to cover their entire body. Don’t forget often-missed areas such as the ears, neck, the back of the hands, and the tops of the feet. For your face, use a nickel-sized amount and be careful around the eyes.
Additional Protective Measures
While sunscreen is a critical component of skin protection, it should be part of a broader sun protection strategy. Wear protective clothing, such as long-sleeved shirts, wide-brimmed hats, and sunglasses. Seek shade during peak sun intensity hours, usually between 10 a.m. and 4 p.m., and be extra cautious near reflective surfaces like water, snow, and sand, which can increase UV exposure.
Special Considerations
Certain activities and environments might require more frequent application or higher SPF levels. For example, high altitudes and tropical regions have stronger UV radiation, necessitating more vigilant sunscreen use. People with fair skin, a history of skin cancer, or certain skin conditions may need to use sunscreen more rigorously and select higher SPF products.
Sunscreen for All Ages
Everyone, regardless of age, should use sunscreen. For children and infants over six months, use a sunscreen specifically formulated for sensitive skin, and consult a pediatrician for advice on sun protection for babies under six months old.
To protect your skin from UV damage, apply broad-spectrum SPF 30 sunscreen daily, even on cloudy or winter days. Apply it at least 15 to 30 minutes before going outside and reapply every two hours, or more often if swimming or sweating. Combine sunscreen use with other sun safety practices for comprehensive skin protection.
Sunscreen Recommendations
How to Treat Actinic Keratosis
Treatment options may include:
- Cryotherapy: The use of liquid nitrogen to freeze the lesions superficially
- Topical Creams: Designed to eliminate Actinic Keratosis in the affected areas.
Featured Products for Sun Protection
Check your local office for current stock!
Check your local office for current stock!
